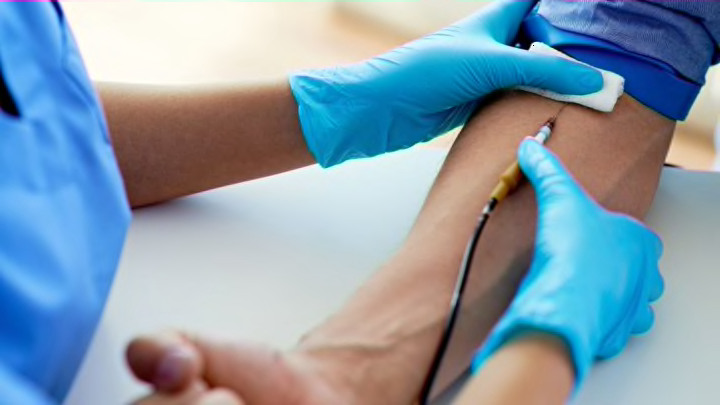
You've rolled up your sleeve, faced a fear of needles, and risked passing out mid-donation. Congrats, you're one of the roughly 6.8 million people who donate blood each year! But even if you've shimmied onto that cot and happily accepted your post-blood draw cookie, you still may have questions about the process. We've answered some of the big ones.
1. Where does the donated blood go?
When you needle up for the American Red Cross, they collect roughly one pint of blood and several test tubes—all of which are stored in iced coolers until they can be transported to an official Red Cross center. From there, the samples are spun in centrifuges to separate the red cells, platelets, and plasma, and the tubes are sent out for testing at one of three national labs.
Samples that come back disease-free are then stored at the center—red cells last in a 6 ºC refrigerator for up to 42 days; platelets remain at room temperature in agitators up to five days; plasma can be frozen for up to a year—until they are shipped to a hospital for use.
2. What do they test for?
Your vials undergo a dozen tests designed to both establish blood type and to weed out donations laced with infectious diseases, such as HIV, hepatitis B and C, and syphilis. If your sample tests positive for something, your donation will be trashed, but on the upside they'll reach out and let you know about your diagnosis and offer counseling with a trained professional.
3. What exactly are platelets, anyway?
Platelets are the tiny, disc-shaped particles inside your blood that help it to clot. They're needed for patients with diseases such as aplastic anemia and leukemia that hamper the body's ability to clot and for patients who are undergoing major surgeries. Platelets are separated from your red blood cells after you donate and can only be stored up to five days. Thus, maintaining a large enough supply can be an issue.
4. How much blood is needed to save a life?
It depends on the situation. According to the American Red Cross, the average red blood cell transfusion is roughly 3 pints, but a single car accident victim could need up to 100 pints.
5. Are certain blood types more valuable than others?

Yes. O positive is the most common blood type in America—belonging to about 38 percent of the population—and thus, the most likely to be needed for a transfusion. (Type A positive ranks second at 34 percent of the population.) O negative blood types—that's about 7 percent of people—are considered the universal donor because their blood can be given to anyone. The least common blood type? AB negative—belonging to just 1 percent of people.
6. How many people donate each year?
Not enough. The American Red Cross estimates that less than 38 percent of the United States population is eligible to donate blood at any given moment—but less than 10 percent of those people do. Each year, roughly 6.8 million donors give 13.6 million units of blood. That may sound like a lot, but approximately 36,000 units are needed across the U.S. each day and because of the short shelf-life, it's difficult to build up an inventory of blood if a lot is needed quickly.
7. Who isn't eligible to donate?
Some states allow 16-year-olds to donate with parental consent, but most require blood givers to be at least 17. You also have to weigh a minimum of 110 pounds and be in good general health. (If you have a cold, flu, or fever, you will be turned away.) Being a world traveler could also be an issue. Those who have recently visited countries where diseases such as malaria or the Zika virus are common are required to wait a set amount of time before offering up a vein. Piercings and tattoos can also temporarily prevent you from donating depending on how long ago you acquired them.
8. Is there any way to speed up the process?
While the Red Cross estimates donating blood can take more than an hour—from the time you fill out your paperwork until you accept the post-donation cookie—you can cut out some time with RapidPass. Users complete forms online, then print them off and bring them to the donation site. For a true walk-in, walk-out experience you can also schedule an appointment. Once you're all set up, the actual blood draw only takes about 10 minutes.
9. How does my body replace the blood lost?
The average adult has between 10 and 12 pints of blood in their body. Since your bone marrow churns out a constant supply of red cells, plasma, and platelets, the plasma you give is replaced within the first 24 hours.
10. Wait, then why do I have to wait 56 days between donations?

While the plasma is replenished quickly, it can take four to six weeks for your body to manufacture the red blood cells that are lost. If you're only donating platelets, which your body replaces within a day, you can give again after a week. However, you're restricted to only 24 total platelet donations a year.
11. Do I need to do anything special after donating?
The American Red Cross suggests replacing the lost iron with foods such as spinach, beans, and red meat as well as drinking an extra 4 to 8 ounces of non-alcoholic liquid. They also advise against doing heavy lifting and recommend keeping your bandage on for at least five hours. (Bonus: that makes it easier to brag to your friends about your largesse!)
12. Why do they ask for my ethnicity?
According to the New York Blood Center, knowing your race makes it easier to match your blood with a needy recipient. "Blood types and antigens are inherited, just like eye and hair color," reads an entry on their website. "Searching for very precise transfusion matches can be like looking for a needle in a haystack, so it makes sense to begin with donors of the same ethnic or racial background as the transfusion recipient." A recent piece in The New York Times concurs: "While no one is suggesting forced segregation of blood bags, it's now scientifically established that blood can be racially or ethnically specific."
13. Can you really make money donating blood?
You can score between $20 and $45 for donating plasma at one of the 530 licensed and IQPP certified plasma collection centers in the U.S., Canada, and Europe. The process is similar to donating blood, except that once the whole blood is drawn, the plasma is separated out and the rest of the blood is returned to your body. (The whole procedure takes between 90 minutes and two hours.) However, this plasma usually doesn't go straight to disease-stricken donees. Instead, it's given to pharmaceutical companies who use it to create medicine for a range of conditions.
14. Can I donate blood to myself?
Yes, but it takes some legwork. You can do what's called an autologous donation—where you donate blood to be used on yourself during a surgery or planned medical procedure—but you'll need a prescription from your doctor.
15. Is there any substitute for blood?
Not yet. However the American Red Cross says they are diligent about tracking research that might help identify an alternative. "The Red Cross actively follows blood substitute research," reads a note on their site, "and works closely with other organizations that develop new transfusion alternatives."
This story was updated in 2019.